Abstract
The Belén District in Loreto Region, Peru, is known for its extensive riverfront areas, where many houses are built on stilts and float during the rainy season. We conducted fecal examinations on 997 schoolchildren (ages 4–14 years; 488 boys, 497 girls) across 4 schools in Belén using the Kato-Katz thick smear and formalin-ethyl acetate sedimentation techniques. The results revealed high rates of soilborne helminths and waterborne protozoan infections, with an overall parasite-positive rate of 79.7%. The primary helminth species were Ascaris lumbricoides (39.2%), Trichuris trichiura (33.2%), Hymenolepis nana (3.4%), hookworms (2.1%), and Enterobius vermicularis (1.5%). The main pathogenic protozoans were Giardia lamblia (20.9%) and Entamoeba histolytica/E. dispar (14.2%), along with Cryptosporidium-like coccidian (4.6%). Non-pathogenic protozoans included Entamoeba coli (31.5%), Endolimax nana (15.1%), and Blastocystis hominis (3.7%). The intensity of soilborne helminth infections was very high for A. lumbricoides (average eggs per gram of feces per child: 18,589), followed by T. trichiura (1,501) and hookworms (160). The prevalence of anemia, often associated with malnutrition, was moderate at 33.1% (298 anemic children among 901 examined). Mass deworming was initiated with albendazole 400 mg, 3 times a year, in conjunction with health education and environmental sanitation. Metronidazole was administered once at a dose of 200 mg 3 times daily for 10 days. A notable finding in this study was that soilborne and waterborne parasites are both highly prevalent among schoolchildren in the floating villages of the Belén District, Loreto Region. Sustained mass deworming is urgently needed and the WASH program is crucial.
-
Key words: Ascaris lumbricoides, Trichuris trichiura, Giardia lamblia, Entamoeba histolytica, Belén District, Peru
Various types of infectious diseases, including viral, bacterial, and parasitic infections, pose major health issues in Peru [
1]. The nationwide prevalence of human immunodeficiency virus is estimated at 0.45%, while tuberculosis affects 117 per 100,000 people, and malaria incidence is 258 per 100,000 [
1]. The population also experiences high rates of diarrheal diseases caused by enteric pathogens, including
Ascaris,
Giardia, enterotoxigenic
Escherichia coli,
Shigella, and
Helicobacter [
1].
Strongyloides stercoralis [
2] and
Cyclospora cayetanensis [
3] are also common diarrheal pathogens in Peru. Consequently, malnutrition, stunting, and anemia are frequent among children in various parts of Peru [
4], especially in the Loreto Region [
5-
10].
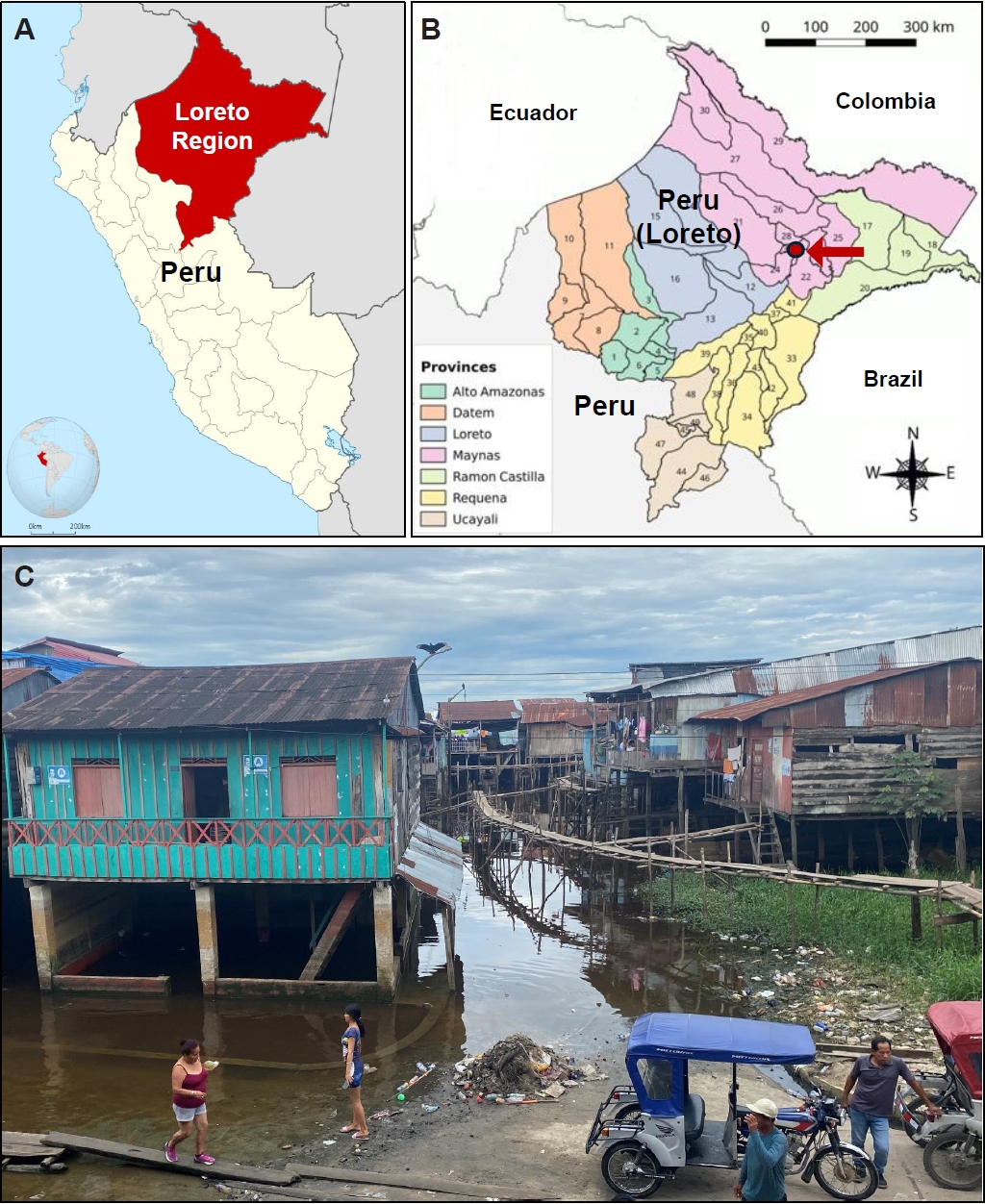
Loreto is the largest department in Peru, covering nearly one-third of the country and the upper parts of the Amazon River (
Fig. 1A,
B). The Belén District in Maynas Province is known for its extensive riverfront areas, where many houses, built on stilts, float during the rainy season (
Fig. 1C), which lasts about 4 to 5 months each year. Residents may be exposed to various soilborne intestinal helminth infections during the dry season (
Fig. 2A,
B) and could be vulnerable to waterborne intestinal protozoans during the rainy season.
The prevalence of soilborne helminthiases has been documented in Belén [
5,
6] and nearby areas, including Mariscal Ramón Castilla, Putumayo, and Requena [
7], as well as Padre Cocha [
8] and Santo Tomás [
9]. However, waterborne protozoan infections are rarely reported in this district, likely due to limited diagnostic capacity and the lack of attention within the local health surveillance system. In June 2024, we examined fecal samples from schoolchildren living in floating villages in Belén and found very high rates of soilborne and waterborne parasitic infections. We also observed that many of these children had anemia, which suggests a long history of malnutrition. In this report, we provide details on intestinal helminthic and protozoan infections, as well as the prevalence of anemia.
Fecal samples were collected from 997 schoolchildren (488 boys, 497 girls, and 12 of unknown sex) from 4 elementary schools in Belén, Loreto Region. The children’s ages ranged as follows: 4–5 years (n=92), 6–7 years (n=192), 8–9 years (n=290), 10–11 years (n=293), 12–14 years (n=99), and unknown age (n=31). Informed consent was obtained from all children, their parents, and/or school guardians.
This project was approved through a memorandum of understanding between Peru and Korea (2024-06-03), signed by Gerencia Regional de Salud (GERESA) and Unidad de Gestión Educativa (UGEL), Loreto, Peru, along with Medipeace Global NGO, Seoul, Korea, and Medipeace Regional Office, Lima, Peru. The title of the project is “Enhancing child health through strengthening intestinal parasite infection management capacity in Loreto, Peru (2024–2026).”
Fecal examinations were carried out using 2 methods [
10]: the Kato-Katz thick smear (
n=982 children) and the formalin-ethyl acetate sedimentation technique (
n=964 children). For each child, one slide sample was prepared with each method and examined microscopically by 5 parasitology experts. To estimate the infection intensity of soilborne helminths, including
A. lumbricoides,
Trichuris trichiura, and hookworms, eggs per gram of feces (EPG) were calculated by multiplying 24 by the number of eggs detected on each Kato-Katz smear for each child, assuming that the fecal volume on each smear is 41.7 g [
10]. The classification of infection intensity followed recommendations from the World Health Organization (WHO) [
11]. In the detection of protozoan cysts/oocysts, special staining techniques, such as Ziehl-Neelsen modified acid-fast staining, were not performed. Molecular genetic techniques were not employed in this study for detecting intestinal helminths or protozoans.
To assess anemia (iron-deficiency anemia), blood samples were collected from 901 schoolchildren, and hemoglobin concentration (Hb, g/dl) was measured using the HemoCue Hb 301 Analyzer (HemoCue). Anemia was defined as a hemoglobin level below 11.5 g/dl for children aged 5–11 years, based on WHO guidelines, and categorized into mild, moderate, and severe anemia for individuals and populations [
12].
Seven species of helminths and 9 species of protozoa were identified. The overall parasite prevalence was unexpectedly high at 79.7% (
Table 1) [
12]. The most common helminth (eggs) was
A. lumbricoides (39.6%), followed by
T. trichiura (33.1%),
Hymenolepis nana (3.4%), hookworms (2.2%),
Enterobius vermicularis (1.5%), small trematode eggs (0.2%), and large trematode eggs (0.1%). The most prevalent protozoan was
Entamoeba coli (31.5%), followed by
Giardia lamblia (20.9%),
Endolimax nana (15.1%),
Entamoeba histolytica (including
E. dispar) (14.2%),
Cryptosporidium-like coccidian (4.6%),
Blastocystis hominis (3.7%),
Iodamoeba bütschlii (2.0%),
Entamoeba hartmanni (1.6%), and
Chilomastix mesnili (1.0%). The number of anemic children was 298 (33.1%) out of 901 examined, which is considered moderate in group anemia level according to WHO guidelines (
Table 1) [
12]. Cases of mild and moderate anemia were observed in 118 (13.1%) and 175 (19.4%) children, respectively, while severe anemia was observed in 5 (0.6%). Age did not show a significant trend in the prevalence of anemia. However, the correlation between current parasitic (helminth or protozoan) infections and anemia was statistically insignificant (
P>0.05, by chi-square tests).
The severity of infection, as indicated by EPGs, varied by soilborne helminth species (
Table 2) [
11]. The proportions of moderate and severe infections with
A. lumbricoides were notably high, at 46.7% and 12.3%, respectively, while the rates for
T. trichiura were lower, at 14.7% and 2.6%. All hookworm cases were mild infections (100%). The average EPG counted 18,589 for
A. lumbricoides, 1,584 for
T. trichiura, and 160 for hookworms.
We consider the overall parasite infection rate of 79.7% in this area to be exceptionally high. It is also noteworthy that both soilborne and waterborne parasitic infections are very common in this region. This appears to be linked to seasonal environmental changes: during the dry season (7 to 8 months each year), the village is exposed to contaminated ground soil with various soilborne helminths, while in the rainy season (4 to 5 months each year), houses float, surrounded by unsanitary water, and are exposed to diverse waterborne pathogens, including intestinal protozoans. Most of the toilet systems in this area are inadequate, which significantly increases the risk of soilborne and waterborne parasitic infections.
Regarding soilborne parasitic infections, several reports have been documented in Belén and its surrounding areas [
5-
9]. In Belén, the prevalence of any helminth infection, including
A. lumbricoides,
T. trichiura, and hookworms, was reported at 37.0% among preschool-age children, which is lower than the 57.6% found in the current study; however, helminth infections in preschool children from this resource-poor community were linked to stunting and anemia [
5]. In another study in Belén, the prevalence of any helminth, including
A. lumbricoides,
T. trichiura, and hookworms, ranged from 72.2% to 78.1% among schoolchildren, which is significantly higher than the 57.6% seen in this study [
6]. In a study conducted across 3 neighboring areas, Mariscal Ramón Castilla, Putumayo, and Requena, the prevalence of any helminth was 49.5%, slightly lower than the prevalence reported here [
7]. However, the prevalence of individual helminth species,
A. lumbricoides,
T. trichiura, and hookworms in these neighboring areas, was 37.2%, 22.8%, and 2.8%, respectively [
7], which is quite similar to the figures in this study: 39.2%, 33.2%, and 2.1%. In Padre Concha, an area adjacent to Belén, the prevalence of
A. lumbricoides was 16.1%, and
T. trichiura was 1.6% among children [
8], substantially lower than in this study. In Santo Thomás, another neighboring area, the prevalence of
A. lumbricoides was 25.2%, and
T. trichiura was 18.5% among preschool children [
9], also lower than the figures reported here.
The infection intensity of
A. lumbricoides was notably high among the schoolchildren surveyed in this study. The average EPG of 18,589 per infected child indicates that the average number of
A. lumbricoides worms infected per child could be as many as 30, based on a previous report in Korea [
13]. Similarly, the average EPG of
T. trichiura was 1,584, suggesting that the worm burden per infected child might reach up to 45 worms, assuming a daily fecal output of 200 g and a daily egg output of 7,000 [
14]. In contrast, the severity of hookworm infection in this region appears to be low, with an average EPG of 160, implying an average worm load of about 3 to 4 worms, assuming a daily egg output of 9,000 [
14].
The widespread presence of intestinal protozoans in this area was previously underreported. It should be noted that
G. lamblia,
E. histolytica, and
Cryptosporidium-like coccidians are well-known pathogenic organisms that can cause diarrhea, malnutrition, and anemia, especially in children [
15]. The cyst stage of
E. dispar, a non-pathogenic amoeba, appears morphologically identical to that of
E. histolytica, but the trophozoite stage of
E. dispar can be distinguished by the absence of red blood cells within its cytoplasm [
15]. In our study,
G. lamblia had a prevalence of 20.9%, which is higher than the 13.7% reported in a previous study conducted among patients with diarrhea in a rural town of the Peruvian Amazon [
16]. However, the 20.9% rate was lower than the 27.9% found in another study focusing on the lowland forest ecoregions of Peru [
17]. The prevalence of
E. histolytica/
E. dispar was 14.2% in this study, while
E. coli, a marker of fecal water contamination, was present at 31.5%. The prevalence of
E. histolytica/
E. dispar in this area was notably lower compared to the 23.8% recently reported from the Amhara region in Ethiopia [
18]. Conversely, the prevalence of
G. lamblia in this study was significantly higher than the 7.3% reported in the same area of Ethiopia [
18]. Therefore, water pollution with intestinal protozoans appears to be a significant concern in this district.
We found that anemia was quite common among the surveyed schoolchildren. The proportion of anemic children in this survey was 33.1%, which is considered a moderate level according to WHO guidelines [
12]. Anemia can result from various conditions, including malnutrition, bleeding, sex (female), infectious diseases, and hematologic or genetic disorders. Therefore, the nutritional status of the surveyed children seems to be poor. However, no statistical significance was noted between the current parasitic infections and anemia. The prevalence of hookworms in our study was 2.2%, which is unlikely to have a significant impact on anemia. However, ongoing and repeated soilborne and waterborne parasitic infections in this area are undoubtedly contributing factors to malnutrition and anemia. Additionally, malaria may also be a contributing factor for anemia, as the Loreto Region has a high endemicity of malaria due to
Plasmodium falciparum and
P. vivax [
19].
Limitations of this study include the lack of special staining, such as the Ziehl-Neelsen technique, for detecting Cryptosporidium-like oocysts. Additionally, molecular methods were not employed to distinguish between E. histolytica and E. dispar infections.
Following this study, mass deworming with albendazole 400 mg in a single dose per child (3 times a year) has been implemented together with health education and environmental sanitation. Mass deworming should continue for at least 10 years or longer to effectively control soilborne helminthiases in this area. Anti-protozoal treatment with metronidazole was also given to those infected with
G. lamblia and/or
E. histolytica/
E. dispar at a dose of 200 mg 3 times daily for 10 days per child. For the management and control of waterborne protozoan infections, the water, sanitation, and hygiene (WASH) program [
20] should be implemented urgently in this area.
Notes
-
Author contributions
Conceptualization: Chai JY, Shin S, Kim SR. Data curation: Chai JY, Kim SR, Lee HR, Kim E. Formal analysis: Chai JY, Kim SR, Kim E. Funding acquisition: Chai JY, Kim SR, Lee S, Shin S, Suh DY. Investigation: Chai JY, Sohn WM, Kim DC, Kim SR, Kim E, Lee HR, Rojas CRT. Methodology: Chang T, Sohn WM, Kim DC, Kim SR. Project administration: Chai JY, Kim SR, Lee S, Shin S, Suh DY, Munayco CV. Supervision: Chai JY, Shin S, Munayco CV. Validation: Chai JY, Kim SR. Visualization: Chai JY. Writing-original draft: Chai JY. Writing- review and editing: Chai JY, Kim SR, Munayco CV.
-
Conflict of interest
Woon-Mok Sohn serves as an editor of Parasites, Hosts and Diseases but had no involvement in the decision to publish this article. No other potential conflicts of interest relevant to this study were reported.
-
Funding
This project is supported by the Korea International Cooperation Agency (KOICA) (2024-2026).
-
Acknowledgments
We thank the staff at the regional reference laboratory of Loreto, Peru, for their assistance with collecting fecal samples from schoolchildren, preparing the Kato-Katz thick smears, and performing the formalin-ethyl acetate sedimentation technique. Medipeace’s health promotion activities in Peru are officially endorsed by the National Superintendency of Public Registries, Peru (operational document No. 2023-4228651).
Fig. 1.The surveyed area in Belén, Maynas Province, Loreto Region, Peru. (A) Map showing the Loreto Region (red color) and Peru. (B) Map showing the Belén District, Maynas Province (red circle, arrowed). Small numbers represent districts. (C) A photo showing a floating village during the rainy season in the Belén District.
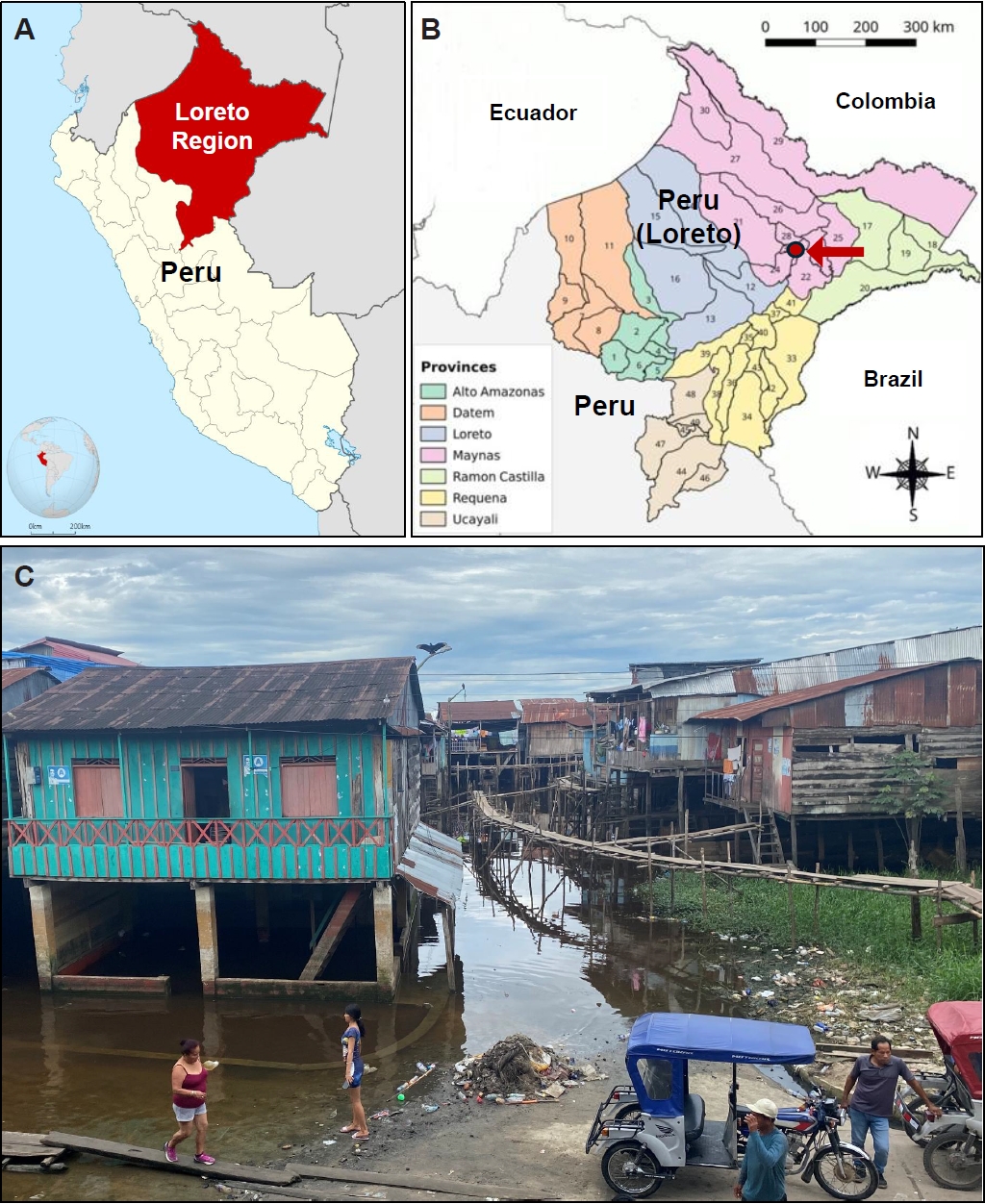
Fig. 2.Photos showing the village of the Belén District, Loreto region, during the dry season. (A) A photo showing a plenty of trashes in a village side. (B) Another village side showing trashes.

Table 1.Prevalence of helminth and protozoan parasites among schoolchildren in the Belén District, Loreto Region, Peru (June 2024)
Table 1.
|
Variable |
No. positive (%) |
|
All parasites |
|
|
No. examined |
997a
|
|
No. positive for any kind of protozoa or helminths |
795 (79.7) |
|
Helminth parasites |
|
|
No. examined |
982 |
|
No. positive for any kind of helminths |
566 (57.6) |
|
Ascaris lumbricoides
|
385 (39.2) |
|
Trichuris trichiura
|
326 (33.2) |
|
Hymenolepis nana
|
33 (3.4) |
|
Hookworms |
21 (2.1) |
|
Enterobius vermicularis
|
15 (1.5) |
|
Small trematode eggsb
|
2 (0.2) |
|
Echinostomatid eggc
|
1 (0.1) |
|
Protozoan parasites |
|
|
No. examined |
964 |
|
No. positive for any kind of protozoa |
542 (56.2) |
|
Entamoeba coli
|
304 (31.5) |
|
Giardia lamblia
|
201 (20.9) |
|
Endolimax nana
|
146 (15.1) |
|
Entamoeba histolyticad
|
137 (14.2) |
|
Cryptosporidium-likee
|
44 (4.6) |
|
Blastocystis hominis
|
36 (3.7) |
|
Iodamoeba bütschlii
|
19 (2.0) |
|
Entamoeba hartmanni
|
15 (1.6) |
|
Chilomastix mesnili
|
10 (1.0) |
|
Hemoglobin level (Hb, g/dl) |
|
|
No. examined |
901 |
|
≥11.5 (no anemia) |
603 (66.9) |
|
11.0–11.4 (mild anemia) |
118 (13.1) |
|
8.0–10.9 (moderate anemia) |
175 (19.4) |
|
≤7.9 (severe anemia) |
5 (0.6) |
|
Total anemicf schoolchildren |
298 (33.1) |
Table 2.Intensity of infection in EPG of soilborne helminths among schoolchildren in the Belén District, Loreto Region, Peru (June 2024)
Table 2.
|
Species of helminth |
No. of children examined |
Mild infection |
Moderate infection |
Severe infection |
Average EPG/infected child |
|
EPG rangea
|
No. (%) |
EPG rangea
|
No. (%) |
EPG rangea
|
No. (%) |
|
Ascaris lumbricoides
|
349 |
1–4,999 |
143 (41.0) |
5,000–49,999 |
163 (46.7) |
≥50,000 |
43 (12.3) |
18,589 |
|
Trichuris trichiura
|
306 |
1–999 |
253 (82.7) |
1,000–9,999 |
45 (14.7) |
≥10,000 |
8 (2.6) |
1,584 |
|
Hookworms |
17 |
1–1,999 |
17 (100) |
2,000–3,999 |
0 (0) |
≥4,000 |
0 (0) |
160 |
References
- 1. Yori PP, Lee G, Olórtegui MP, et al. Santa Clara de Nanay: the MAL-ED cohort in Peru. Clin Infect Dis 2014;59 Suppl 4:S310-6. https://doi.org/10.1093/cid/ciu460
- 2. Otero-Rodriguez S, Casapia-Morales M, Pinedo-Cancino V, et al. High prevalence of Strongyloides stercoralis in people living with HIV: a critical health challenge in the Peruvian Amazon Basin. PLoS Negl Trop Dis 2025;19:e0013231. https://doi.org/10.1371/journal.pntd.0013231
- 3. Mundaca CC, Torres-Slimming PA, Araujo-Castillo RV, et al. Use of PCR to improve diagnostic yield in an outbreak of cyclosporiasis in Lima, Peru. Trans R Soc Trop Med Hyg 2008;102:712-7. https://doi.org/10.1016/j.trstmh.2008.03.003
- 4. Cabada MM, Goodrich MR, Graham B, et al. Prevalence of intestinal helminths, anemia, and malnutrition in Paucartambo, Peru. Rev Panam Salud Publica 2015;37:69-75.
- 5. Gyorkos TW, Maheu-Giroux M, Casapía M, Joseph SA, Creed-Kanashiro H. Stunting and helminth infection in early preschool-age children in a resource-poor community in the Amazon lowlands of Peru. Trans R Soc Trop Med Hyg 2011;105:204-8. https://doi.org/10.1016/j.trstmh.2010.12.003
- 6. Gyorkos TW, Maheu-Giroux M, Blouin B, Casapia M. Impact of health education on soil-transmitted helminth infections in schoolchildren of the Peruvian Amazon: a cluster-randomized controlled trial. PLoS Negl Trop Dis 2013;7:e2397. https://doi.org/10.1371/journal.pntd.0002397
- 7. Saboyá-Díaz MI, Carey Angeles CA, Avellaneda Yajahuanca RDS, et al. Associated factors of the co-occurrence of trachoma and soil-transmitted helminthiases in children 1 to 9 years old in rural communities of the Amazon basin in Loreto Department, Peru: results from a population-based survey. PLoS Negl Trop Dis 2022;16:e0010532. https://doi.org/10.1371/journal.pntd.0010532
- 8. Errea RA, Vasquez-Rios G, Calderon ML, et al. Soil-transmitted helminthiasis in children from a rural community taking part in a periodic deworming program in the Peruvian Amazon. Am J Trop Med Hyg 2019;101:636-40. https://doi.org/10.4269/ajtmh.18-1011
- 9. Segoviano-Lorenzo MDC, Trigo-Esteban E, Gyorkos TW, et al. Prevalence of malnutrition, anemia, and soil-transmitted helminthiasis in preschool-age children living in peri-urban populations in the Peruvian Amazon. Cad Saude Publica 2022;38:e00248221. https://doi.org/10.1590/0102-311XEN248221
- 10. World Health Organization. Bench aids for the diagnosis of intestinal parasites. 2nd ed. The Organization; 2019.
- 11. World Health Organization. Helminth control in school-age children: a guide for managers of control programmes. 2nd ed. The Organization; 2011.
- 12. World Health Organization. Guidelines on haemoglobin cutoffs to define anaemia in individuals and populations. The Organization; 2024.
- 13. Chai JY, Hong ST, Lee SH, Seo BS. Fluctuation of the egg production amounts according to worm burden and length of Ascaris lumbricoides. Korean J Parasitol 1981;19:38-44. https://doi.org/10.3347/kjp.1981.19.1.38
- 14. Seo BS. Clinical parasitology. Il Cho Kak; 1978.
- 15. Garcia LS. Diagnostic medical parasitology. 6th ed. ASM Press; 2016.
- 16. Yori PP, Schwab K, Gilman RH, et al. Norovirus highly prevalent cause of endemic acute diarrhea in children in the Peruvian Amazon. Pediatr Infect Dis J 2009;28:844-7. https://doi.org/10.1097/INF.0b013e3181a24730
- 17. Cabrera R, Whittembury A, Terashima A. Prevalence of Giardia lamblia by ecoregions in Peruvian preschoolers and school-aged children: risk stratification proposal. Annals Fac Med 2023;84:168-76. https://doi.org/10.15381/anales.v84i2.25351
- 18. Hailu T, Alemu G. Prevalence of Entamoeba histolytica/dispar and Giardia lamblia infections and their associated factors among schoolchildren in the Amhara region, Northwest Ethiopia. Food Waterborne Parasitol 2024;36:e00241. https://doi.org/10.1016/j.fawpar.2024.e00241
- 19. Mousam A, Maggioni V, Delamater PL, Quispe AM. Using remote sensing and modeling techniques to investigate the annual parasite incidence of malaria in Loreto, Peru. Adv Water Resour 2017;108:423-38. https://doi.org/10.1016/j.advwatres.2016.11.009
- 20. McMichael C. Water, sanitation and hygiene (WASH) in schools in low-income countries: a review of evidence of impact. Int J Envron Res Public Health 2019;16:359. https://doi.org/10.3390/ijerph16030359
 , Woon-Mok Sohn2
, Woon-Mok Sohn2 , Dong-Chan Kim3
, Dong-Chan Kim3 , Sehyeon Regina Kim4
, Sehyeon Regina Kim4 , Eunseo Kim4
, Eunseo Kim4 , Hae Ram Lee5
, Hae Ram Lee5 , Sangmi Lee5
, Sangmi Lee5 , Sangmoon Shin5
, Sangmoon Shin5 , Dong Youb Suh5
, Dong Youb Suh5 , Cesar Renato Tuesta Rojas6
, Cesar Renato Tuesta Rojas6 , César Vladimir Munayco7
, César Vladimir Munayco7